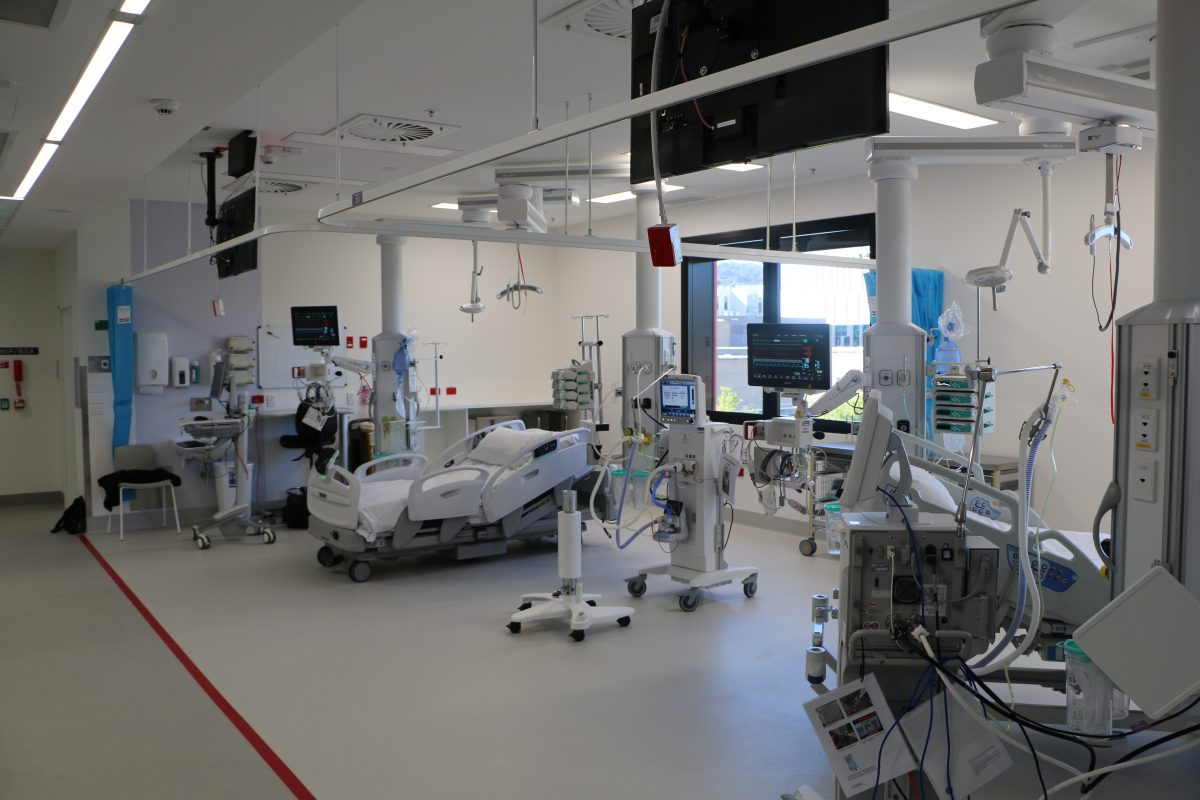
Yesterday, 80 people were in the Territory’s hospitals with the virus. Five were in the ICU (pictured) and two required ventilation. Photo: ACT Government.
Since the beginning of the year, 47 Canberrans have died ‘with’ COVID-19. To yesterday (17 May), there have been 59 deaths related to the virus since the beginning of the pandemic.
They are sobering facts.
And every time a death is reported, a question is raised: why do we report deaths ‘with’ COVID-19 and not deaths ‘from’ COVID-19?
What’s the quick answer?
Unfortunately, there really isn’t one.
Using ‘with’ makes things easier for health authorities as there’s an agreed-upon set of reporting guidelines.
In the future, it will also make it easier for researchers to learn more about the pandemic.
But it’s also partly because understanding a cause of death can be quite complicated. This is particularly true if the person who died was elderly and/or had underlying health conditions.
What do we know about COVID-19 deaths already?
Of the 2639 Australian COVID-19 deaths reported to the Australian Bureau of Statistics before 31 January 2022, nearly all of them (2556; 97%) have been directly linked to the virus.
But 91 per cent of these deaths occurred in people who had at least one other health condition and the median age for a COVID death was 83.7 years old.
What’s the current definition of a COVID death?
At this point in the pandemic, all states and territories are following national guidelines for defining and reporting COVID deaths.
The Federal Department of Health defines a COVID-19 death as a death of a person who is either a confirmed or probable COVID-19 case.
But they do not attribute death to COVID-19 if there is a clear alternative – such as if a person tested positive for the virus but then was involved in a major car accident.
In cases where a person has had a ‘distinct period of recovery’ between illness and death, that shouldn’t be counted as a COVID death either.
Who determines cause of death?
It’s up to the medical practitioner, or in some cases the coroner, to determine the primary cause of death, as well as any contributing factors.
All of these are listed on that individual’s death certificate. ACT Health says if COVID-19 is written as either the primary cause of death or a contributing factor, that death is noted and reported as a COVID death.

In years to come, experts will look back on the pandemic and see what more can be learned. Photo: Michelle Kroll.
What do the experts say?
For elderly people, one infectious diseases expert said COVID-19 is often the “straw that breaks the camel’s back”.
“When you’re in your 80s or 90s you might have heart disease, lung disease or cancer, as well as COVID-19 – so which do you attribute the cause of death to?” asks ANU Medical School Professor Peter Collignon.
“That’s when things get complex because, at some point, you have to attribute the death to these things proportionately. So it’s easier to say ‘with’ rather than ‘from’ because you can’t look at every death individually yet.”
So, if COVID-19 isn’t the ‘smoking gun’, why is it important we know about the deaths?
Well, Professor Collignon says it’s not okay to simply stop reporting deaths – complicated and complex as the data may be – as it may downplay the role of COVID-19 in the person’s death.
In the future, it’s likely we will be able to put a number on the number, or percentage of deaths, which were caused by COVID-19 or were hastened by it.
Will we learn more in the future?
In all likelihood, the answer is yes, as experts just like Professor Collignon will undertake research into the pandemic.
If that data isn’t collected now, this will never be able to happen.
It’s also not the first (and probably won’t be the last) time studies like this will be conducted.
By way of an example, two decades ago, Professor Collignon was involved in a study which looked at people who died with Staphylococcus aureus (often referred to as ‘staph’ or ‘golden staph’) in the bloodstream. Like COVID-19, lots of the people who died had underlying health conditions.
To work out how a person died, researchers had to assess whether or not they believed a person would still have been alive in 12 months had they not contracted staph. Similar questions may be asked about COVID-19 deaths.

Remember the days of checkpoints at the Territory’s borders? Photo: Michelle Kroll.
Is this just about public health?
No. This is also complicated (but if you’ve followed the ‘with’ and ‘from’ argument closely, you knew that already). After all, it’s now been more than two years of lockdowns, border closures, emergency declarations, mandates, masks, checking in, working from home, learning from home (and much more). The pandemic has impacted much more than health.
As Professor Collignon puts it: “it’s controversial, it’s political and it’s emotional … so we need to know more.”
Original Article published by Lottie Twyford on Riotact.